Tens of thousands of organ transplants each year save many lives. However, problems sometimes arise, such as complications and graft rejection, which can make it difficult to complete the procedure successfully in the long term. Research indicates that THA can help prevent immune rejection of the graft.
Organ transplants continue to save thousands of lives around the world every day, but guaranteeing a successful outcome is not always easy (https://medlineplus.gov/ency/article/000815.htm). The main problem is that our bodies are set up to use the immune system to defend against any external threats, including transplanted organs. The immune system can trigger a transplant rejection reaction, which can lead to fatal outcomes (https://www.sciencedaily.com/releases/2015/09/150901113535.htm).
However, a 2015 study by Nagarkatti and colleagues suggests that tetrahydrocannabinol (THC) may help prevent rejection of transplanted organs or tissues in rodents. THC is one of the best known and most studied cannabinoids responsible for many of the physical and psychoactive effects of cannabis.
The legalization of medical and recreational cannabis is becoming a hot topic in many countries around the world. Some of them have already passed laws, while others are in the decision-making stage or are just beginning discussions on the subject.
More and more studies are appearing every day, confirming and illuminating the many medical and therapeutic benefits of cannabis (https://www.nccih.nih.gov/health/cannabis-marijuana-and-cannabinoids-what-you-need-to-know).
Such studies can allay the fears of those who continue to express opposition to cannabis legalization. They also emphasize the need for additional research to be developed in order to conduct such studies in a clinical setting with human participants.
Some of the recent research is related to surgery. In this article, we will specifically focus on one of the most compelling studies published in 2015, which adds another benefit to the already extensive list of properties of cannabis and, in particular, THC.
What is the therapeutic value of THC?
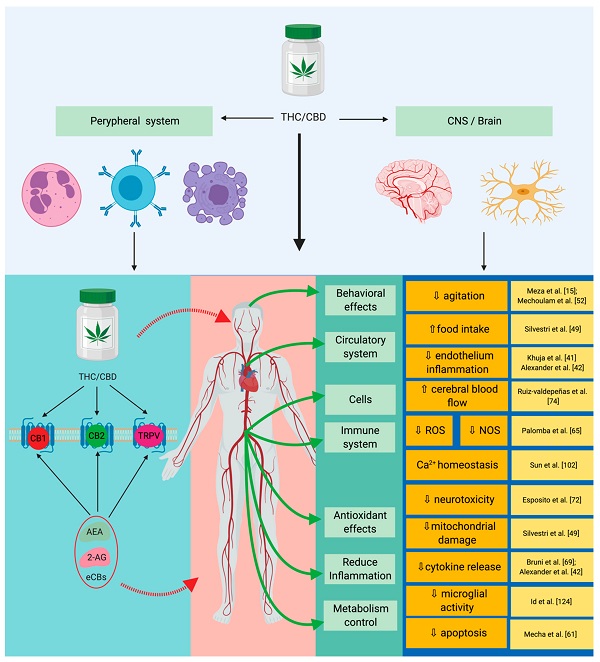
In 2015, a team of scientists from the University of South Carolina School of Medicine published a study looking at the effects of THC on skin grafts. According to the study, tetrahydrocannabinol (THC), a key cannabis compound, may help slow rejection in patients with incompatible organ transplants by activating cannabinoid CB1 receptors in immune cells.
“A growing body of research is pointing to possible beneficial effects of components in marijuana, but the main challenge is identifying the molecular mechanisms involved,” John Verry, deputy editor of the Journal of Leukocyte Biology, said in a statement (https://academic.oup.com/jleukbio/article-abstract/98/3/435/6936024?redirectedFrom=fulltext).
THC’s ability to control the immune system was first identified in the 1970s (https://link.springer.com/chapter/10.1007/978-1-4615-1951-5_15). After a series of tests in rodents, the results demonstrated that THC could improve the results of organ transplants by suppressing the immune response that leads to rejection of transplanted organs.
As a result, more lives can be saved through transplantation. Clearly, this is further evidence of the significant therapeutic potential of cannabis. This is especially true for THC, which along with CBD is the most studied natural cannabinoid.
What is an organ transplant?
Organ transplantation represents one of the most important examples of scientific development in modern medicine. When organs or tissues stop functioning due to disease, it may be necessary to replace the diseased organ or tissue. This requires a donor and also requires that the recipient’s immune system does not cause rejection.
Among the most commonly transplanted organs and tissues are kidneys, liver, heart, and bone marrow. While some organs (e.g., heart) can only be donated after the donor dies, others (e.g., kidney, liver, and bone marrow) can be donated by living donors.
Statistics around the world speak for themselves. Every day hundreds of thousands of people are waiting for organ transplants, thousands of whom die without waiting for the necessary organ to survive (http://www.transplant-observatory.org/). One donor can save up to eight lives, so one person can donate eight organs. Approximately 10% of potential recipients die while waiting for an organ transplant (https://www.organdonor.gov/statistics-stories/statistics.html).
Why does graft rejection happen?
Each person has an individual immune system that depends on both genetics and the environment. This system helps protect us against disease by recognizing foreign bodies and infectious agents. Such agents can be contagious, such as bacteria or viruses, but so can cells from another person whose immune system and individual response are very different from ours.
Nuclear cells have markers on their surface which, after inoculation or transplantation into another organism, are recognized as foreign. These markers are called histocompatibility antigens and they give each person’s tissues unique characteristics that distinguish them from others.
Our innate immunity protects us perfectly and is characterized by:
-
A quick first line of defense response (e.g., the skin, our largest organ) against infectious agents.
-
The ability of the immune system to stimulate non-specific immune cells working to destroy potentially harmful substances entering the body.
When an invasion becomes so severe that the innate immune system cannot handle it, our “adaptive immunity” comes to the rescue (https://www.ncbi.nlm.nih.gov/books/NBK21070/). Adaptive immunity is characterized by a more specific, slower and longer-term response of specialized cells, such as T cells and B cells, to external agents. This is the type of immunity that is activated when a transplant is rejected.
Although organ and tissue transplants are now helping to prolong human life more than ever before, there are risks involved. One major problem arises when the recipient’s immune system, in particular his T cells, recognizes the new donor organ as “foreign” and begins to attack it.
For this reason, it is important that the recipient’s immune system be as similar as possible to that of the donor, which can be very difficult to coordinate, given how unique each person’s immune system is, and the speed at which organ failure can lead to death.
And this is where THC comes to the rescue.
How to avoid transplant rejection?
Before a tissue transplant, a study must be performed to determine whether the antigens it contains are compatible with the recipient, thus avoiding rejection. Although tissue testing ensures that the transplanted organ or tissue is as similar as possible to the recipient’s organ or tissue, there is no 100% compatibility.
Each person has unique antigens that are different from others, except for identical twins. This is why it is necessary to use immunosuppressants that suppress our immune system so that the body does not trigger an immune response and attack the foreign tissue.
In the first year after transplantation, about 25% of kidney recipients and 40% of heart recipients experience episodes of acute rejection (https://med.stanford.edu/news/all-news/2010/09/researchers-find-faster-less-intrusive-way-to-identify-transplant-recipients-organ-rejection.html). However, although these episodes do not always result in the loss of an organ, they require immediate intervention.
Modern immunosuppressive therapy can successfully treat more than 90% of cases of acute rejection (http://www.med.umich.edu/trans/public/pdf/6_Medications.pdf). However, it is important to note that immunosuppressive drugs used to prevent transplant rejection can have harmful side effects. These effects may include:
-
Diarrhea
-
Hypertension
-
Acne
-
Weight gain
-
High cholesterol
-
High blood sugar
-
Susceptibility to infection
-
Dental problems
Considering all of these factors, in addition to the fact that the demand for organs far exceeds the available supply, and that most patients often have only one chance to receive a donor organ or tissue, transplant rejection can have devastating consequences that can lead to death.
Can THC prevent graft rejection?

For his study, Nagarkatti used mice that had undergone skin grafting surgery. The skin of one group of mice was transplanted into another group of genetically different mice. The incompatible skin was treated with either a placebo or the active compound cannabis, THC.
The researchers injected donor spleen and skin cells into the recipient mice, using the rodents as models for human organ transplants. The study found that recipient mice who received THC were less likely to reject the new tissue than those treated with placebo. The study showed that THC helped prevent rejection through several mechanisms by activating CB1 receptors:
-
Preventing an increase in the number of T-cell receptors in the recipient’s lymph nodes, thereby reducing the likelihood of donor tissue rejection
-
Effects on reducing inflammatory response signals
-
Stimulating myeloid suppressor cells that reduce the T-cell receptor response and prevent rejection.
-
Increased survival time of skin cells from donors
It is important to recall a previous study published in 2013 in the online journal Journal of Pharmacology Neuroimmune (http://link.springer.com/article/10.1007/s11481-013-9485-1). That study suggested how THC could stop the immune response that causes rejection of transplanted organs, in this case through CB2 receptors.
Although only cell culture models were used in this study, the researchers observed a dose-dependent effect: higher doses of THC led to higher levels of immunosuppression. In addition, two synthetic cannabinoids were included in the study, and it was found that they could work just as well.
The researchers concluded that cannabinoids hold great promise for improving organ transplant success based on these results.
Research results
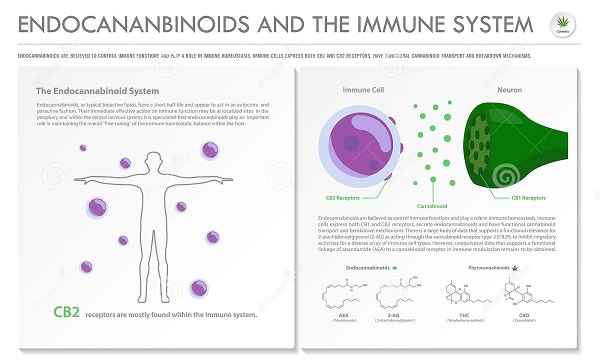
The University of South Carolina conducted a study that confirms the usefulness of cannabinoids in modulating and reducing inflammatory processes (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4469415/). These processes are associated not only with transplant rejection, but also with autoimmune disorders, cancer and other serious diseases.
The study showed that cannabinoid receptors can provide a new treatment for graft versus host reactions and prevent allograft rejection by suppressing the immune response in the recipient. This discovery could have important implications for the development of new treatments for serious diseases.
Given the serious side effects associated with current treatments used to prevent transplant rejection, as well as the very favorable safety profile of THC, the authors say that more effective treatments with fewer side effects are badly needed. Unfortunately, advances in cannabis-based medicine appear to be due to the development of synthetic compounds rather than purely scientific discoveries.
“These data support the potential of this class of compounds as a useful therapy to prolong graft life in transplant patients” – said Mitzi Nagarkatti.
Are there any downsides?

Ironically, even though the THC content of medicinal cannabis can help transplant patients, in many fears medical cannabis patients may be denied organ transplants. Even those who use cannabis to treat many conditions or relieve their symptoms and test positive for cannabis may be denied. This is especially surprising when it happens in the United States, where medical cannabis is legal in many states.
Various cases have been published in the media, such as that of a 64-year-old patient named Norman Smith. He was told that his doctors would remove him from the list of patients to be transplanted if he did not stop using cannabis for at least six months.
They also required that he participate in a substance abuse treatment program during this period. Ironically, he was prescribed medicinal marijuana at that medical center to help him cope with the side effects of chemotherapy for liver cancer. Unfortunately, Mr. Smith died before he was reinstated to the transplant waiting list.
Dr. Colquhoun stated that they should take substance abuse issues seriously because they often play a role in the development of diseases that may require transplantation and may adversely affect the new organ after transplantation. However, this claim is not supported by scientific evidence, given that cannabis use does not cause organ dysfunction.
In addition, to consider the use of herbal medicine to alleviate pain from incurable illness as a substance abuse problem is probably a mistake on the part of the medical professional. These claims seem to be based on stigma and ignorance.
Unfortunately, such decisions can have fatal consequences on the lives of innocent people who are sick and need a transplant just as much as other patients in the same situation. Especially considering that a 2009 study showed that cannabis users and non-cannabis users had similar survival rates after a liver transplant, and that current substance abuse policies do not systematically put marijuana users at additional risk of death.
Eight U.S. states now prohibit the denial of organ transplants based on cannabis use. However, according to Legacy Health spokesperson Piset Peach, the fight to prevent discrimination against cannabis users in Oregon continues, and it is difficult to determine a specific number of patients who may be less likely to receive a transplant based on one factor alone.
Clearly, the current policy on the legality of medical cannabis, which prohibits access to health care for these people, needs to be changed. Policymakers might do the right thing by adopting the experience of California, which has passed a law to protect such patients.
Conclusion
There is a clear need for further and deeper research into the usefulness of THC in preventing rejection in humans. It is sad that this has not yet been done, given that the usefulness of THC in preventing transplant rejection was discussed as early as 1974.
The potential of THC in this area should be explored to prolong and save even more lives around the world – lives that are being given a second chance thanks to the altruistic donations made by thousands of people who care. Lives that, thanks to THC, have been able to overcome the terrible prospect of rejection after a much-needed transplant.