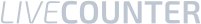The number of people with autism, a neurological developmental disorder, continues to grow. Affected individuals have difficulty interacting socially and communicating (https://www.webmd.com/brain/autism/understanding-autism-basics#1). Cannabis may represent a promising treatment option, as a 2019 Israeli study confirms, which is consistent with anecdotal evidence gathered over the years. However, many questions remain unanswered.
Autism or autism spectrum disorders (ASDs) are complex developments affecting the brain. There are many forms of the disorder that cause problems in the following aspects:
- interaction with others (social interaction)
- Verbal and nonverbal communication
Repetitive and stereotypical behaviors, interests and actions are also characteristic of this condition. Asperger’s syndrome is a form of autism in which cognitive development and speech are not impaired.
Autism is much more common than many people assume. According to the World Health Organization (WHO), 1 in 160 children has ASD, although other sources indicate much higher rates (https://www.who.int/news-room/fact-sheets/detail/autism-spectrum-disorders). Nevertheless, the dramatic increase in the number of autism diagnoses worldwide is an undeniable fact.
Both genetic and environmental factors are thought to contribute to the development of autism, but a comprehensive model of explanation has not yet been developed.
Treating autism with cannabis
ASD is an incurable condition, but there are various therapies that can improve the quality of life of people with autism. These include cognitive, psychological and pedagogical approaches.
More and more patients using cannabis in treatment are expressing support for its use (https://www.healthline.com/health/can-autism-be-cured). Several years ago, famous author Marie Myung-Ok Lee spoke openly about cannabis as a treatment for her son with autism (www.independent.co.uk/life-style/health-and-families/features/the-ultimate-herbal-remedy-can-cannabis-improve-autism-1814756.html):
«Marijuana is not a panacea for autism, but in our son’s case it significantly reduces pain and inflammation, allowing him to participate and learn again. It also protects him from the sometimes dangerous side effects of medications. We chose the right variety (White Russian, the preferred analgesic for patients with terminal cancer) and dosage. Now that the pain is gone, D. can go to school instead of the child psychiatric hospital where many of his peers end up due to aggressive behavior».
Adjunct professor of psychiatry and doctor emeritus at Harvard Medical School, Dr. Lester Greenspoon, published an article on cannabis use in autism in 2010 (www.beyondthc.com/wp-content/uploads/2013/08/GrinspoonAutism.pdf).
In that article, Dr. Greenspoon details the experience of Marie Myung-Ok Lee, who uses medical marijuana to treat her son, J.J. The professor urges scientists to scrutinize the experience and conduct more research on drug treatments:
«Anecdotal evidence gets less attention than before, but it is the source of much of our knowledge about synthetic and plant-based medicines. Controlled experiments were not required to recognize the therapeutic potential of chloral hydrate, barbiturates, aspirin, curare, insulin, or penicillin».
In addition to Marie Myung-Ok Lee’s report, there are reports of many other children whose autism symptoms decreased after taking medical cannabis. For example, Calel Santiago (www.inquisitr.com/2170618/kush-cannabis-oil-cure-a-9-year-old-boy-with-severe-autism-says-his-first-words-after-medical-marijuana-treatment/) allegedly spoke his first words after taking CBD. As with epilepsy, most parents choose to give CBD oil to their children with autism, which seems to have positive results. If cannabinoid receptor activation during a child’s growth is one of the causes of autism disorders, it is also important to consider whether using antagonists such as CBD can stop this effect.

In some cases reported in the media, the combination of THC and CBD has proven to be more effective. According to reports, children with epilepsy and autism disorder benefit the most from increased THC (https://www.collective-evolution.com/2015/02/17/what-happened-when-they-treated-autistic-children-with-medical-cannabis/). There is also a study on a six-year-old boy with autism whose symptoms improved significantly after treatment with dronabinol, a synthetic analog of THC (https://cannabis-med.org/data/pdf/en_2010_04_1.pdf).
Alan Flashman, who has successfully used medical marijuana to treat more than 500 children with autism in Israel, shares his opinion on the optimal ratio of THC to CBD (https://blogs.timesofisrael.com/cannabis-and-autism-an-informal-update-2019/):
«The results are very consistent. As I mentioned, about 60% of children respond well to oil with a 20:1 ratio (CBD to THC). Another 15-20% need a higher THC content, often higher than CBD. The remaining 20% continue to raise some questions for me; sometimes changing cannabis varieties plays a big role. But sometimes you have to admit that the treatment has not been effective».
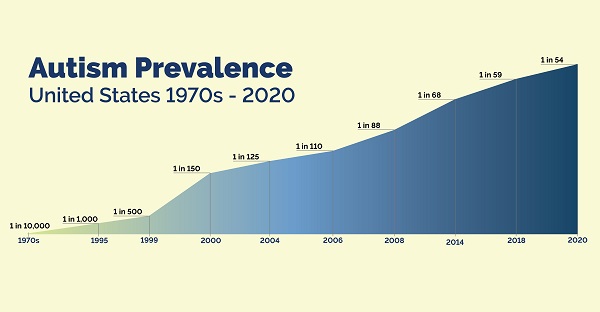
ECS is directly related to autistic disorders

Over the past few years, remarkable research findings related to autism disorders and the endocannabinoid system have been published. The areas of the brain with the highest concentrations of CB1 receptors have been found to be those presumably dysfunctional in autism, including the cerebellum, hippocampus, and basal ganglia (https://www.ncbi.nlm.nih.gov/pubmed/15749244).
During human embryonic development, CB1 receptors and their associated endocannabinoids play important roles in neuronal differentiation and axonal migration; both processes are necessary for normal neurological development (https://www.ncbi.nlm.nih.gov/pubmed/19647111). Other studies suggest that CB1 receptors may be responsible for determining the position of synapses. Thus, one theory is that activation of CB1 receptors in childhood may trigger autistic disorders because they interfere with normal brain development.
Role of CB2-receptors in autistic disorders
CB2 receptors may also play a role in autistic disorders. CB2 receptor agonists have been shown to reduce the frequency with which certain key immune cells, such as monocytes, infiltrate the endothelium, the thin layer of cells that separates the circulation from tissues and organs (https://www.ncbi.nlm.nih.gov/pubmed/17660390). Monocytes are among the key cells associated with the immune system, and disruption of their development and function has been repeatedly observed in the context of autism disorders (www.jimmunol.org/content/192/1_Supplement/52.25).
A 2013 study showed that CB2 receptor concentrations in monocytes were elevated in children with autism, while concentrations of CB1 receptors and the anandamide reducing molecule fatty acid amide hydrolase (FAAH) remained unchanged (link.springer.com/article/10.1007/s10803-013-1824-9).
The role of the dopamine system in autism

One study on the subject describes the case of a middle-aged man who had previously been diagnosed with schizophrenia. Because of his psychotic symptoms, he sought emergency psychiatric care, where he was first diagnosed with Asperger’s syndrome. Schizophrenia and Asperger’s syndrome share many similar characteristics, leading to their confusion.
After therapy with the antipsychotic Aripiprazole, the symptoms of Asperger’s syndrome improved significantly (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2654534/).
Aripiprazole acts as a partial dopamine D2-receptor agonist, and there is strong evidence for a link between schizophrenia, Asperger syndrome, and dopamine dysfunction.
In addition, anandamide is thought to play a role in this process. Anandamide is known to be involved in the dopamine signal exchange system, although the exact mechanism cannot yet be fully understood. Nevertheless, studies suggest that one of the many functions of anandamide in the central nervous system may be to modulate psychomotor and social activity, carried out primarily through the dopamine receptor D2 (https://www.ncbi.nlm.nih.gov/pubmed/10777802).
The role of genes in the development of autism

Previously, it was thought that 90% of autism cases were due to genetic factors. However, it is now assumed that this estimate was too high because it was based on insufficient high-quality studies of twins, and the actual inheritance of autism is only 50% (https://jamanetwork.com/journals/jama/fullarticle/1866100).
X-Linked Chromosome Syndrome, a form of autism, is the most common monogenic (https://www.nature.com/articles/nm.3127) (that is, associated with a single gene or chromosome mutation) form of inherited autism and is caused by inactivation of the FMR1 gene responsible for producing the FMR protein. The endocannabinoid system is known to be involved in the regulation of cognitive functions such as anxiety, pain perception, seizure predisposition, and synaptic plasticity (the ability of synapses to increase or decrease their activity depending on their degree of use), and all these characteristics are impaired in X chromosome fragility syndrome.
One study examining the role of the endocannabinoid system in male mice lacking the FMR1 gene during reproduction showed that blocking CB1 receptors normalized cognitive impairment, pain perception and seizure susceptibility, while blocking CB2 receptors normalized anxiety.
Research confirms that cannabis relieves symptoms of autism
As noted earlier, many patients express support for the use of cannabis to treat symptoms of ASD. However, it is worth bearing in mind that these are individual results, not confirmed by rigorous empirical studies that exclude the influence of other factors on the effect obtained (https://www.apa.org/monitor/2015/11/marijuana-brain).
Such data are not sufficient to recommend medical cannabis preparations containing THC to children, especially considering the concerns about the effects of THC on brain development. In addition, different forms of autism respond differently to THC intake, and more research is needed to more accurately determine this response (https://www.nature.com/articles/s41598-018-37570-y).
A 2019 study from Israel gives reason for optimism. Researchers from Ben-Gurion University of the Negev (BGU) and Soroka University Medical Center confirm that cannabis is well tolerated, safe and effective for treating symptoms of PAS. This may be a starting point for future research.