Glaucoma is a common eye condition that affects millions of people worldwide, and if left untreated, it can lead to blindness. While traditional treatments for glaucoma include medication and surgery, recent research has suggested that THC, the main psychoactive component in cannabis, may also be an effective treatment option. THC has been found to lower intraocular pressure, a key factor in the development and progression of glaucoma. This article will explore the potential benefits of THC for glaucoma patients, as well as the potential risks and side effects associated with this treatment option.
What causes glaucoma?
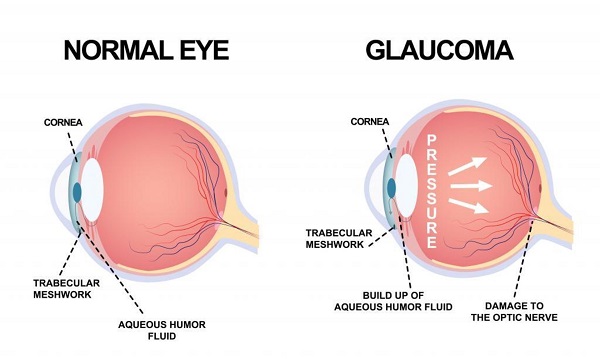
Glaucoma is a condition that occurs when there is damage to the optic nerve, which is responsible for transmitting visual information from the eye to the brain. In most cases, this damage is caused by increased pressure inside the eye, known as intraocular pressure.
The eye constantly produces a fluid called aqueous humor, which helps maintain the shape of the eye and provides nutrients to the surrounding tissues. Normally, this fluid drains out of the eye through a network of small channels. However, in some people, these channels become blocked, causing the fluid to accumulate and leading to increased intraocular pressure. This increased pressure can damage the optic nerve over time, leading to vision loss or even blindness.
Other risk factors for glaucoma include age, family history, and certain medical conditions such as diabetes and high blood pressure.
Types of glaucoma
There are several types of glaucoma, each with its own unique characteristics and risk factors. The following are the most common types of glaucoma:
- Primary Open-Angle Glaucoma (POAG):This is the most common type of glaucoma and affects millions of people worldwide. In POAG, the drainage canals in the eye become clogged over time, leading to increased pressure in the eye and damage to the optic nerve. POAG often has no symptoms in its early stages and can only be detected through regular eye exams.
- Angle-Closure Glaucoma: This type of glaucoma occurs when the iris (the colored part of the eye) blocks the drainage canals, leading to a sudden increase in eye pressure. Symptoms of angle-closure glaucoma can include severe eye pain, nausea, and vision loss. This type of glaucoma requires immediate medical attention to prevent permanent vision loss.
- Normal-Tension Glaucoma: In this type of glaucoma, the optic nerve becomes damaged even though eye pressure remains within the normal range. The exact cause of normal-tension glaucoma is not fully understood, but it may be related to poor blood flow to the optic nerve.
- Congenital Glaucoma: Congenital glaucoma is a rare type of glaucoma that occurs in infants and young children. It is typically caused by an abnormality in the eye’s drainage system and can cause symptoms such as excessive tearing, sensitivity to light, and cloudiness in the eye.
- Secondary Glaucoma: This type of glaucoma occurs as a result of another eye condition, such as inflammation or injury. It can also be caused by certain medications, such as steroids, that increase eye pressure.
Regular eye exams are essential for detecting glaucoma early and preventing vision loss.
How does the weed affect glaucoma?

Marijuana has been a topic of interest in the treatment of glaucoma for many years.
Marijuana, or cannabis, has been found to lower intraocular pressure (IOP) by reducing the production of aqueous humor, the fluid that circulates in the eye and maintains eye pressure. It achieves this by activating cannabinoid receptors in the eye, which causes a relaxation of the smooth muscle tissue in the eye’s ciliary body, allowing the aqueous humor to flow more easily out of the eye.
Several studies have shown that marijuana can lower IOP by up to 25% in some people. However, the effect is generally short-lived and typically lasts for only a few hours. Moreover, the amount of marijuana required to achieve a significant reduction in IOP can cause unwanted side effects, such as dry mouth, dizziness, and impaired cognitive function.
In addition to its effects on IOP, marijuana can also cause changes in blood pressure and heart rate, which can lead to further complications in people with glaucoma. Furthermore, smoking marijuana can actually increase IOP in some people, especially when used in high doses or for long periods of time. This is because smoking can cause blood vessels in the eyes to dilate, leading to an increase in pressure.
Why is cannabis not a good remedy for glaucoma?
For these reasons, the American Academy of Ophthalmology does not recommend marijuana as a primary or secondary treatment for glaucoma. Instead, they recommend using proven therapies such as eye drops, laser treatment, or surgery to lower IOP and prevent further optic nerve damage.
It is important to note that marijuana may interact with other medications and can have negative effects on overall health, particularly in those with underlying medical conditions. Therefore, individuals with glaucoma should always consult with their healthcare provider before using marijuana or any other alternative treatments.
Does THC lower eye pressure?
THC (tetrahydrocannabinol), which is the primary psychoactive component of marijuana, has been found to lower IOP in some people with glaucoma.
Studies have shown that THC can lower IOP by up to 25% in some individuals with glaucoma. However, the effect is typically short-lived and may only last for a few hours. Moreover, the amount of THC required to achieve a significant reduction in IOP can cause unwanted side effects.
It is important to note that while THC may be effective in reducing IOP, it is not recommended as a primary or secondary treatment for glaucoma. This is because the effect is temporary, and the risks of long-term marijuana use may outweigh the benefits.
Glaucoma medicines

There are several types of medications that are commonly used to treat glaucoma. These medications work by either decreasing the production of aqueous humor (the fluid that circulates in the eye) or increasing its outflow, which helps to lower intraocular pressure in the eye. Some of the most commonly used glaucoma medications include:
- Prostaglandin analogs: These medications work by increasing the outflow of aqueous humor from the eye. They are typically given as eye drops once daily and include drugs such as latanoprost, bimatoprost, and travoprost.
- Beta blockers: These medications work by decreasing the production of aqueous humor. They are typically given as eye drops and include drugs such as timolol, betaxolol, and carteolol.
- Alpha agonists: These medications work by decreasing the production of aqueous humor and increasing its outflow. They are typically given as eye drops and include drugs such as brimonidine and apraclonidine.
- Carbonic anhydrase inhibitors: These medications work by decreasing the production of aqueous humor. They are typically given as eye drops or oral tablets and include drugs such as dorzolamide, brinzolamide, and acetazolamide.
- Rho kinase inhibitors: These medications work by relaxing the smooth muscle tissue in the eye, which helps to increase the outflow of aqueous humor. They are typically given as eye drops and include drugs such as netarsudil.
- Combination medications: These are medications that contain two or more different types of glaucoma medications in a single eye drop. They are typically used when one medication alone is not sufficient in lowering IOP.
It is important to note that all medications have potential side effects, and it is important to discuss the risks and benefits of each medication with a healthcare provider before starting treatment. Additionally, medications should be used as directed and regularly monitored to ensure they are effectively lowering IOP and preventing further optic nerve damage in people with glaucoma.
Laser surgery for glaucoma
Laser surgery is one of the treatment options for glaucoma that is used to lower intraocular pressure in the eye. The goal of laser surgery for glaucoma is to increase the outflow of aqueous humor (the fluid that circulates in the eye) to decrease IOP and prevent further optic nerve damage. There are several types of laser surgeries used for glaucoma, including:
- Selective laser trabeculoplasty (SLT): SLT uses a low-energy laser to target the trabecular meshwork, which is the drainage system of the eye. This procedure helps to improve the outflow of aqueous humor and can reduce IOP. SLT is typically performed in an outpatient setting and does not require any incisions or stitches.
- Laser peripheral iridotomy (LPI): LPI is used to treat narrow-angle glaucoma, which is a less common form of glaucoma. This procedure involves using a laser to create a small hole in the iris, which helps to improve the flow of aqueous humor and reduce IOP. LPI is typically performed in an outpatient setting and does not require any incisions or stitches.
- Cyclophotocoagulation (CPC): CPC uses a laser to target the ciliary body, which is responsible for producing aqueous humor. This procedure reduces the production of aqueous humor and can help to lower IOP. CPC is typically reserved for people with advanced glaucoma who have not responded to other treatments.
Laser surgery for glaucoma is generally considered safe and effective, with a lower risk of complications compared to traditional glaucoma surgeries. However, like all procedures, there are potential risks and side effects, including temporary inflammation, bleeding, and blurred vision.
Microsurgery and minimally invasive surgeries
Microsurgery and minimally invasive procedures are also options for the treatment of glaucoma, particularly for those with moderate to severe disease that has not been successfully controlled with medication or laser therapy. These surgical techniques can help to lower IOP and prevent further optic nerve damage.
Some examples of microsurgery for glaucoma include:
- Trabeculectomy: This procedure involves creating a small flap in the sclera (the white part of the eye) to allow fluid to drain out of the eye and lower IOP. A small bubble called a bleb is formed under the conjunctiva (the thin layer that covers the white part of the eye) and helps to regulate the flow of fluid out of the eye.
- Glaucoma drainage implants: These devices are small tubes that are inserted into the eye to help drain excess fluid and lower IOP. There are several types of implants available, including the Ahmed valve, Baerveldt implant, and Molteno implant.
Minimally invasive glaucoma surgeries (MIGS) are newer surgical techniques that use smaller incisions and have a shorter recovery time compared to traditional glaucoma surgeries. Some examples of MIGS procedures include:
- iStent: This tiny device is implanted during cataract surgery and helps to improve the outflow of fluid from the eye, lowering IOP.
- Trabectome: This procedure involves using a tiny probe to remove a portion of the trabecular meshwork, which helps to increase the outflow of fluid from the eye.
- Canaloplasty: This procedure involves using a microcatheter to dilate and unblock the natural drainage pathway in the eye, allowing for improved fluid outflow and lower IOP.
Microsurgery and minimally invasive procedures for glaucoma are generally safe and effective, with a lower risk of complications compared to traditional surgeries. However, it is important to discuss the risks and benefits of these procedures with a healthcare provider before undergoing any surgery.
Summary
THC has been shown to lower intraocular pressure in people with glaucoma. However, the effect is short-lived and tolerance to the drug’s effects can develop quickly. Additionally, the side effects of THC, such as decreased blood pressure and increased heart rate, can be problematic for some patients, particularly those with cardiovascular or respiratory issues. While THC may be useful as an adjunct therapy for some people with glaucoma, it is not considered a first-line treatment and should only be used under the guidance of a healthcare provider. Other treatment options, such as medications, laser surgery, and microsurgery, are more effective at reducing IOP and preventing further optic nerve damage. It is important for individuals with glaucoma to work with their healthcare provider to develop an individualized treatment plan that takes into account their medical history and specific needs.